WHAT IS THE HALO TECHNOLOGY?
The technology consists of two different devices; the HALO360+ ablation catheter and the HALO90 focal ablation device. The balloon-based HALO360+ device is capable of treating larger areas of circumferential Barrett’s esophagus, while the focal ablation device is used to treat smaller areas.
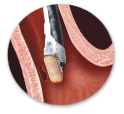
ABLATION WITH HALO 90
The HALO90 focal ablation device is designed to treat small areas of Barrett’s esophagus, independently or in conjunction with the HALO360 System.
BEFORE TREATMENT
“Ablation” (or coagulation) is a technique where tissue is heated until it is no longer viable or alive. Physicians have used various forms of ablation for nearly a century to treat a number of cancerous and precancerous conditions, as well as to control bleeding. The HALO ablation technology is a very specific type of ablation, in which heat energy is delivered in a precise and highly-controlled manner.
Barrett’s esophagus tissue is very thin and is therefore a good candidate for removal with ablative energy. Delivery of ablative energy with the HALO ablation technology is therefore capable of achieving complete removal of the diseased tissue without damage to the normal underlying structures.
Ablation therapy is performed in conjunction with upper endoscopy. The treatment is performed in an outpatient setting and no incisions are involved. A patient should ask the physician or nurse for more information on where the procedure is performed and the time required for the procedure.
DURING THE PROCEDURE
Using standard endoscopy techniques, the physician activates and controls the different functions of the HALO90 System.
- The ablation catheter is first mounted onto the endoscope.
- Both devices are introduced into the esophagus.
- By manipulating the endoscope, the ablation catheter is positioned within the esophagus at the affected portion of the esophagus.
- The physician delivers ablative energy to the targeted tissue. The energy application is less than 1 second and is delivered in an automated manner. The design of this technology limits the energy delivery to a depth clinically shown to remove the diseased tissue (less than 1 mm) while reducing the risk of injury to the deeper tissue layers.
- For patients with more than one lesion of Barrett's esophagus, the HALO90 Ablation Catheter is repositioned and the ablation steps are repeated.

AFTER TREATMENT-WHAT TO EXPECT AFTER THE PROCEDURE?
Patients may experience chest discomfort, pain, and difficulty swallowing for several days after the procedure, all of which are managed with medications provided by the physician, these symptoms typically resolved within 3-4 days. Patients are provided with anti-acid medications to promote healing of the treated esophagus and replacement of the diseased Barrett’s tissue with a normal, healthy esophagus lining.
It is very important that a patient follows the discharge instructions provided by the physician or the nursing staff after the procedure to ensure limited time of discomfort and ensure proper healing of the esophagus. Clinical studies show that regrowth of healthy tissue occurs within one month in the treated area.
A follow-up appointment is scheduled within 2-3 months to assess the response to treatment. If there remains any residual Barrett’s tissue, additional therapy may be recommended.
Clinical studies have demonstrated the Barrett’s tissue can be completely eliminated with the HALO ablation technology in 98.4% of patients.
HOW IS GERD MANAGED AFTER A SUCCESSFUL ABLATION?
Successful elimination of the Barrett’s esophagus tissue does not cure pre-existing GERD or the associated symptoms. You must continue to take the recommended Acid Reflux Therapy prescribed by your physician to prevent the regrowth of Barrett's Esophogus cells.
After Radiofrequency Ablation Treatment, you will be instructed to take a special regimen of your PPI or Acid Reflux medication to control the excess acid while the ablated tissue is healing. You will be given a medication called "GI Cocktail, that should be taken four times daily or 30 mins prior to any meal. The GI cocktail is a combination of liquid antacid and liquid lidocaine that will make the ablated area less sensitive to food and liquids.
On the day of the procedure you will be instructed to have only liquids such as soup broth, milkshakes, Ensure, ect. You will also be instructed to avoid certain foods and liquids for the few weeks. You will be instructed to gradually increase your diet to soft foods such as; pudding, mashed potatoes, yogurt, pasta, ect. The ablated tissue must be given time to heal, hard solid foods may cause injury to healing tissues.
You will also be instructed to avoid aspirin and nonsteroidal anti-inflammatory medications for 7 days.




